My initial intent for writing these newsletters was to talk about public health research and measures to prevent common illnesses—not just discuss COVID-19 related topics—however, I feel there is a need to share certain information and clarify COVID-19 topics that are easily misinterpreted or misinforming. I promise the next topic will be something new and different!!!
Read my previous newsletter on the COVID-19 vaccine side effects here.
If I’m being honest, I had never heard of coronavirus until the pandemic hit, and once I learned more about it through objective research and in my biology classes, it is a lot more prevalent than one might think.
There are seven coronaviruses known to impact humans.
Coronaviruses are a type of virus, and there are thousands that exist, some of which can cause diseases (the SARS-CoV-2 causes COVID-19 illness, for example). They are divided into four subgroups: alpha, beta, gamma, and delta.
There are four known coronaviruses that circulate through the human population—
HCoV-NL63 (alpha coronavirus)
HCoV-229E (alpha coronavirus)*
HCoV-OC43 (beta coronavirus)*
HCoV-HKU1 (beta coronavirus)
*we have known about these two in particular for a long time
These four viruses are thought to cause some of the common colds that are seen in humans today; 10%-15% of common cold symptoms are caused by these four.
More recently, there are three beta coronaviruses that have emerged either through a species acting as an intermediate host or zoonotic transfer—
SARS-CoV-1 (first reported in 2002)
MERS-CoV (first reported in 2012)
SARS-CoV-2 (first reported in 2019)
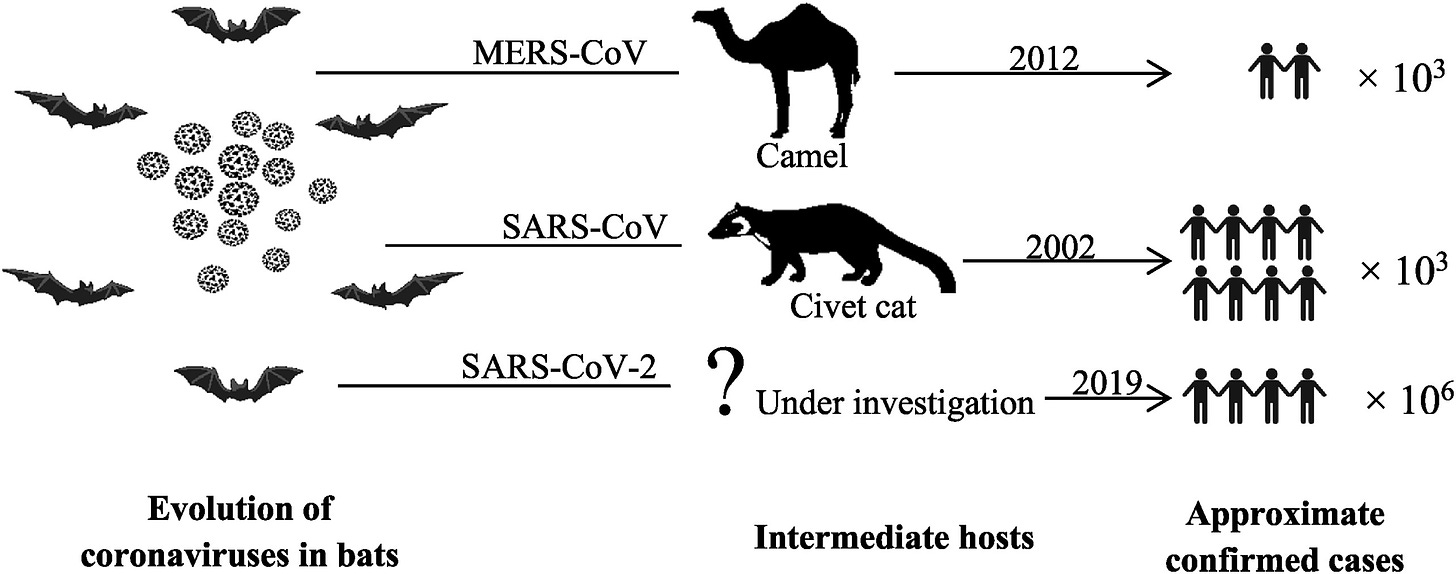
These three are also thought to originate from bats, like many other coronaviruses, however they are different from the gamma and delta coronaviruses which have common ancestors in birds. While SARS 1, MERS, and SARS 2 likely emerged from bats, they were transmitted to humans from an intermediate host. For SARS 1, the intermediate hosts are thought to be civet cats; for MERS, the intermediate hosts are probably dromedary camels. Once infected in these animals, replications occur within them which lead to mutations, allowing the virus to spread to humans. It is still unknown if SARS 2 has an intermediate host(s) and which animal that could be.
Image source
In China, there are 500 identified coronaviruses in bats and over 5,000 unidentified diverse coronaviruses. Because there have been three pathogenic coronaviruses that have surfaced in less than 20 years, scientists believe that it is extremely likely more coronaviruses will appear and affect the human population. When the pandemic ends, it does not necessarily suggest that doctors, scientists, virologists, and just all humans can completely forget about coronaviruses and the study of them because based on the trajectory of the three most recent viruses, more occurrences will likely happen in the future.
Comparing the pathogenic zoonotic coronaviruses
SARS-CoV-1
SARS 1 first emerged in 2002 in southern China with 8,096 cases and 774 total deaths. This was an epidemic that lasted a year.
MERS-CoV-1
MERS first emerged in 2012 in the Arabian Peninsula, causing 2,574 cases and 886 total deaths. This virus is the most infectious of all the viruses, with the highest death rate of 34%. Unlike SARS 1, MERS infections still occur but it is unlikely to circulate through the human population. MERS does not spread easily from human to human, which is why there are very few cases reported; new infections that occur are likely spilled over from dromedary camels to humans.
One might ask why then was the SARS 1 epidemic contained in less than a year whereas the current SARS 2 pandemic is still ongoing? There are three main reasons for this:
The origin for SARS 1 was known—civet cats. Thus, the chain of transmission could be broken knowing where the virus was coming from. In 2004, the CDC banned the importation of civet cats and that ban is still in place today. The main reservoir or intermediate host is still not known for SARS 2.
Human transmission for SARS 1 mainly occurred in hospital settings, and thus medical personnel were informed immediately of this risk and protocols were put in place to contain the virus. With SARS 2, there is not just widespread transmission in hospitals but also in all communities throughout the world.
Most notably, SARS 1 did not transmit until 24-36 hours after symptoms with very few asymptomatic cases. For SARS 2, the case is completely opposite. There are many mild or asymptomatic cases that can go undetected and lead to people unknowingly infecting others.
Origins of SARS-CoV-2
New articles and studies have come out that beg the question of whether or not COVID-19 came from a lab. It’s consequential to word this correctly because it can be easily misinterpreted. Scientists and researchers can confidently say that SARS-CoV-2 did derive from nature/bats. There is no question regarding this, because the genomic structure of SARS 2 was sequenced, and it is extremely similar to other coronaviruses in nature. If it had been created by humans, then one of the several genetic systems for beta coronaviruses would have been used, but the genetic data shows the virus backbone of SARS-CoV-2 is not from anywhere else. Read about that finding here. However, it is plausible that the virus spilled over from a lab that was studying it—not engineered by humans for intentional use. After the SARS 1 epidemic, the Wuhan labs started collecting coronavirus samples to conduct further research. Someone who was studying it could have accidentally left the lab unknowingly contracting it and passed it on to those around him. The WHO is still doing research to officially understand where it likely came from or if there is an intermediate host. Saying that it came from a lab without providing further context is extremely detrimental to the public’s view of science and their understanding of the pandemic overall.
Immunity to SARS-CoV-2
Scientists know that the SARS 1 immunity response was short lived; the initial neutralizing antibody response was strong, but it did not last long. For most people, the response disappeared a few years post infection. This was worrisome for scientists, and they tried to understand what that meant for immunity to SARS 2 since it is much more widespread.
New studies reported in the NY Times just came out confirming that immunity to SARS 2 lasts up to a year and will improve significantly after vaccination. These studies suggest that those who recovered from SARS 2 and were later immunized will likely not need a booster shot. Those who were never infected and receive a vaccine will likely need booster shots as well as those were still infected but did not produce enough of an antibody response.
All of the information regarding the history of coronaviruses was gathered from a lecture by University of California - Berkeley virologist and professor, Dr. Britt Glaunsinger. I highly suggest you watch the entire video below if you want to learn about the scientific and genetic details of SARS-CoV-2.
Disclaimer: All information in my newsletters are for educational purposes only. Please consult with your healthcare provider or a medical professional if you have any questions or concerns.
Thank you so much for reading.
Please email me at reemlfawaz@gmail.com if you have any questions!